IVF patients have many reasons to consider embryo genetic testing
In the early years of in vitro fertilization, embryologists were trained to rate embryos by how they looked under a microscope. Differences in how embryologists were trained, individual interpretations and multiple rating systems around the world, however, made it difficult to determine what a “good” embryo really was. In other words, “how likely will this embryo make a healthy baby?” was perceived differently by embryologists.
Today, thanks to advanced embryo genetic testing, we now have impressive technology that can determine if the embryo is genetically normal. Specifically, preimplantation genetic testing for aneuploidy, PGT-A, has revolutionized IVF since its introduction several years ago. PGT-A biopsies a few of cells from the outer layer of an embryo to determine if it is chromosomally healthy with the right number of chromosome pairs that it inherited from its mother and father. The embryo is then classified as euploid (normal) or aneuploid (abnormal).
Since embryo aneuploidy is a major cause of non-implantation or early miscarriage during an IVF cycle (and natural cycles, for that matter), the ability to screen an embryo before transfer to the uterus has prompted monumental changes in fertility treatment. Being able to select for transfer an embryo that has the best odds of implantation has had three major, interlocking effects on IVF. All three reasons to consider embryo genetic testing have made IVF safer, more successful, and decreased the overall time to a pregnancy.
Three reasons you should consider embryo genetic testing
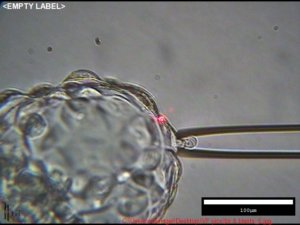
First, euploid embryo selection has allowed reproductive endocrinologists to decrease the number of embryos transferred at any one time. Today, almost all transfers are just one embryo, down from the two to three that was common just a few years ago. This has drastically decreased the number of higher order pregnancies such as twins and triplets, decreasing birth complications for a huge impact on the health of the baby and the mom. Our own twin pregnancy rate has decreased from 51% in the early 2010’s to just around 1% today.
Second, because the euploid embryo has a greater chance of survival, IVF success rates have shot up from a national average of 35% to around 55% now. At Fertility Answers, our own pregnancy rates with biopsied embryos have increased to greater than 60%. Compared to all other forms of assisted reproduction, IVF with PGT-A brings about success rates that even Mother Nature can’t compete with.
And third, embryo biopsy has helped significantly with family planning and overall time to pregnancy. Imagine a couple with three frozen embryos awaiting eventual transfer – two are abnormal and not compatible with life and one is normal. Just a few years ago, this couple would not have been able to know that two of their embryos had little chance of implantation. They likely would have gone through three embryo transfers. Transferring the abnormal embryos risked either not getting pregnant or a miscarriage, which carries a very real emotional, financial, and physical toll. With PGT-A, we are able to avoid transferring embryos that have no chance at pregnancy, selecting the best embryos first and achieving a pregnancy up to four months faster based on prior studies.
PGT-A results in safer pregnancies, better outcomes, and faster conception
Overall, embryo biopsy using PGT-A leads to better outcomes, safer pregnancies, and faster results, especially in advanced maternal age patients or in patients at higher risk of miscarriage. At Fertility Answers, we are happy to offer this option to improve their chances. Contact us if you have questions about reasons to consider embryo genetic testing.


